Artificial feeding in emergencies: experiences from the ongoing Syrian crisis
 By Suzanne Mboya
By Suzanne Mboya
Suzanne Mboya is a consultant nutritionist. In 2014 she completed a sixth month mission supporting the Syrian crisis IYCF-E response through a partnership agreement between Save the Children Jordan and the UNICEF Jordan country office, with financial support from the UNICEF Middle East North Africa Regional Office.
Suzanne acknowledges and thanks the UNICEF regional team, country specific offices and Save the Children teams in Jordan and at headquarters.
The views expressed in this article are the author’s own and do not necessarily reflect those of UNICEF and Save the Children.
This article describes elements of the infant and young child feeding response in the Syrian crisis and the author’s perspective on the major issues arising from it, with particular consideration of challenges around artificial feeding. It draws on the findings of a six month UNICEF/ Save the Children Jordan mission to support optimal IYCF practices and take account of the IYCF in emergencies (IYCF-E) response1. It is accompanied by five case studies of individual mothers compiled by the author during her time in the region, to give an insight into the complexities and realities around infant feeding in the crisis.
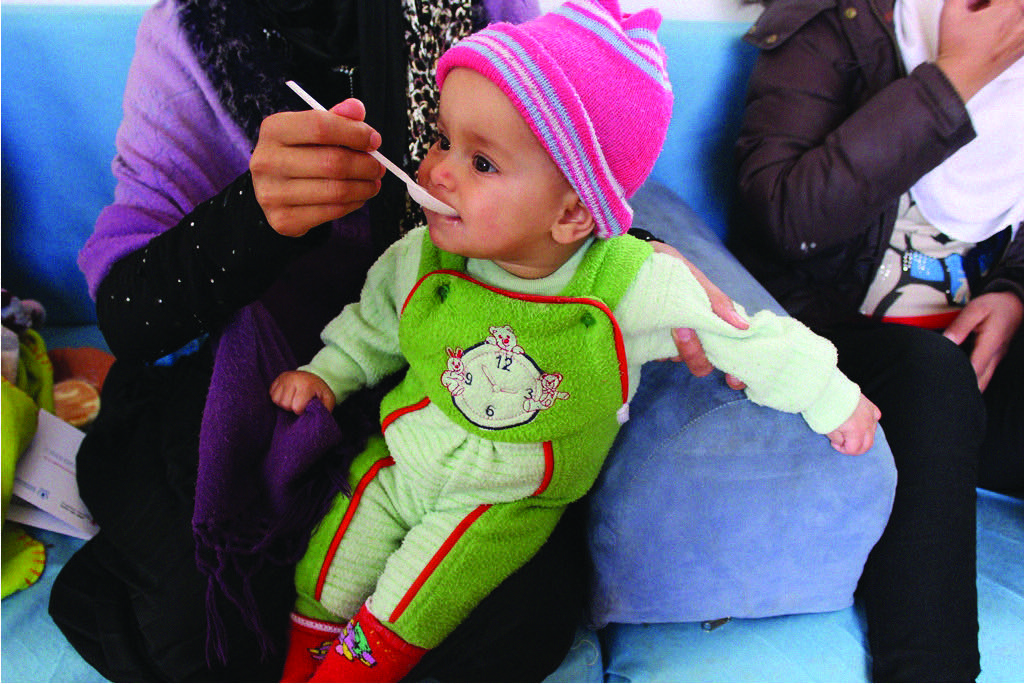 Context
Context
The provision of infant formula and milk for infants and young children during emergencies remains a very controversial subject. Humanitarian aid agencies have continued to struggle with how to tackle this problem since the early 1990s, when emergency responses in countries such as Iraq and Lebanon revealed that a significant percentage of women had been using breastmilk substitutes (BMS), typically infant formula, before the crises hit. Previously, relief work had focused on countries where the pre-crisis breastfeeding rate was nearly 100%; although breastfeeding practices were often less than ideal, at least that lifeline for infants was there.
The recurring challenges in infant feeding during emergencies over the last decade or more prompted agencies to develop infant and young child feeding in emergencies (IYCF-E) policies, initiatives and training materials. However, the ongoing conflict in Syria has again highlighted the difficulties in supporting formula-fed infants, while at the same time promoting breastfeeding.
According to the Syrian Family Health Survey (SFHS) (2009), conducted prior to the crisis, the nutrition situation of children under five years of age was poor, with an estimated 23% stunted, 9.3% wasted and 10.3% underweight. Exclusive breastfeeding rates stood at 42.6% while the proportion of newborns introduced to breastfeeding within the first hour was 42.2%. Micronutrient deficiencies were also recorded in Syria, presenting risk of sub-optimal growth among children, e.g. anaemia prevalence among 0-59 month old children was 29.2%2, Vitamin A deficiency rate was 8.7%3 and iodine deficiency prevalence was 12.9%4
At time of writing, more recent IYCF data from Syria are not available but a rapid nutrition assessment conducted in August 2013 revealed that many women in Syria are misinformed about the ability of mothers to breastfeed during the current crisis and that the exclusive breastfeeding rate is decreasing5,6. Lack of privacy and lack of time were cited as barriers to exclusive breastfeeding. This is exacerbated by the fact that some local and international non-governmental organisations (NGOs) are importing BMS and providing it in a way that is undermining breastfeeding and increasing infants’ risk of diarrheal diseases, malnutrition and death.7,8
Policy guidance & regulation
Two important policy guidance are the International Code of Marketing of Breastmilk Substitutes (the Code) and the Operational Guidance on IYCF-E; both are endorsed in World Health Assembly Resolutions (see Box 1). Based on an overall analysis of IYCF indicators and efforts being made to improve them, Syria is considered a ‘category 2’ country by the International Baby Food Action Network (IBFAN)9 in that there are laws that partly comply with the Code. For example, whilst the Code states there should be no promotion of BMS9, bottles and teats in any part of the health care system, the Syrian law permits promotion of BMS if the Ministry of Health (MOH) gives approval10. BMS were widely used in Syria before the crisis. Infant formula (a nutritionally appropriate BMS) was manufactured in Damascus and imported through Latakya. It was then provided to pharmacies throughout Syria where it could be purchased. The Drug and Food Standards Authority Institute of the Government of Syria controlled the distribution of infant formula11.
Box 1: International policy guidance on IYCF-E
The International Code of Marketing of Breastmilk Substitutes is an international health policy framework for breastfeeding promotion adopted by the World Health Assembly (WHA) of the WHO in 1981. The Code applies in both emergency and development contexts. The Code was developed as a global public health strategy and recommends restrictions on the marketing of BMS, such as infant formula, to ensure that mothers are not discouraged from breastfeeding and that substitutes are used safely if needed. The Code also covers ethical considerations and regulations for the marketing of feeding bottles and teats. A number of subsequent WHA resolutions have further clarified or extended certain provisions of the Code, including around emergencies. On its own, the International Code is not legally enforceable. Companies are only subject to legal sanctions for failing to abide by the Code where it has been incorporated into the legislature of a nation state. Access at: http://ibfan.org/code-monitoring/114
The Operational Guidance on Infant Feeding in Emergencies provides concise guidance for emergency relief staff on how to ensure appropriate infant and young child feeding in emergencies. It is produced and managed by a collaboration of NGOs, UN agencies and individual experts (IFE Core Group). First produced in 2001, it has been updated in 2004 and 2007 in response to lessons from emergency experiences. Sphere IYCF Standards (2011) are based on its recommendations. It is available in 13 languages. Access at: http://www.ennonline.net/operationalguidanceiycfv2.1
 Violations of the Code (and non-compliance with the Operational Guidance on IYCF-E) during the response in Syria have been noted and include:
Violations of the Code (and non-compliance with the Operational Guidance on IYCF-E) during the response in Syria have been noted and include:
- Foreign governments mainly from the Gulf region have donated infant formula, bottles and pacifiers to the health care system in both community and refugee camps with packaging sometimes not in Arabic (violation of Code 1994, non-compliance with Ops Guidance on IYCF-E 6.4.2; Violation of Code Article 9.2 and non-compliance with Ops Guidance on IYCF-E 6.3.6).
- NGO’s distribute ‘baby kits’ including infant formula and bottles to hospitals, municipalities and directly to refugee and IDP households (Untargeted distribution is a violation of Code Article 6.6 and non-compliance with Ops Guidance on IYCF-E 6.4.1 and 6.4.3).
- Single tins of infant formula (defined as ‘samples’ by the Code) are distributed to mothers by health workers (violation of Code Article 7.4) without undertaking that the supplies would continue for as long as the infant concerned needed them (violation of Code Article 6.7 and non-compliance with Ops Guidance on IYCF-E 6.3.5).
- Tins of formula milk received by NGOs as donations are in a foreign language (violation of Code Article 9.2 and non-compliance with Ops Guidance on IYCF-E 6.3.6).
Arising challenges
The direct and indirect effects of the ongoing Syrian crisis have heightened the vulnerability of mothers and children to undernutrition. The types of IYCF-E interventions implemented to widely varying degrees in the Syria response are listed in Box 2.
Box 2: Emergency interventions to promote, protect and support optimal infant feeding in the Syria response
- Revitalisation and adoption of mother and child friendly related policies and guidelines
- Individual and community level counselling on safe infant feeding practices
- Establishment of mother/baby friendly spaces
- Bottle exchange programmes (where feeding bottles are exchanged for cups)
- Prescription and provision of infant formula
- In a few settings, monitoring violations of the Code
- Blanket distribution of ready-to-use foods for children and women to boost their micronutrient status and prevent malnutrition
- Micronutrient supplementation of mothers and children with iron-folic acid supplements, vitamin A supplements and deworming tablets
- Close monitoring of the situation including nutrition screening on arrival and periodically in the community, nutrition assessment, etc.
The prolonged conflict in Syria has caused a disruption of supply networks and market systems, including for infant formula. Although breastfeeding remains the preferred mode of feeding, particularly for babies up to the age of six months, there are some situations in Syria where breastfeeding is not a viable option. Mothers who had already made an informed choice not to breastfeed now have babies dependent on infant formula but are no longer able to access supplies. This has resulted in use of non-milk substitutes, including herbal drinks, tea and sugar-water to feed babies and infants exacerbating the problems of malnutrition12. In addition, babies and infants who have lost their mothers in the conflict are being cared for by relatives and friends, making maternal breastfeeding impossible. Whilst re-lactation remains the first option for the non-breastfed infants, the absence of skilled lactation support in Syria means there is no support to help caregivers’ initiate/practice re-lactation. Very limited and intermittent access across borders and between governorates makes assessments and the estimation of non-breastfed infants in need of support difficult. Internally displaced people who are living in besieged areas within Syria beyond the reach of international aid agencies are mostly affected.
“ One thing that is of concern is the number of requests on the internet and social media from individuals’ and charities for the donation of ‘formula milk’ for babies from individuals and charities within the region.” Umm Nasayba, UK based columnist
Providing support to IYCF in a crisis is a relatively new concept for countries in the Middle East such as Jordan and Turkey which are host countries to fleeing refugees. What it entails is little understood, even by health and nutrition staff. Most NGOs and front-line relief workers believe that IYCF-E is only about promoting breastfeeding and thus is not highly prioritised in early phase of emergencies. In countries such as Iraq, Lebanon and Syria, where many women use infant formula in non-emergency settings and “know how to do it”, many people fail to understand why infant formula should not be freely distributed during an emergency. Is it time to re-consider infant and young child feeding guidelines in urban settings where pre-crisis practices indicate infants were predominantly formula fed.
Agencies recognise the significant importance of breastfeeding to the health and wellbeing of infants and are mindful of the need to ensure that the supply and distribution of infant formula does not undermine the health benefits of breastfeeding. NGOs have adopted and endorsed statements in line with the position of the United Nations (UN) and the World Health Organisation (WHO) on infant feeding in refugee settings, the international conventions on breastfeeding, including the Code and the Operational Guidance on IYCF-E13. However infant formula prescription, dispensing and follow up remain a major challenge for aid workers and partner agencies. Although artificial feeding was established in Syria before the crisis, the current artificial feeding situation is unclear due to lack of documentation on the numbers and locations of non-breastfed infants, on the situation regarding BMS use and on complementary feeding for non-breastfed infants. Some agencies do not document for fear of criticism for not upholding the Operational Guidance on IYCF-E;
“We sometimes distribute infant formula to non-breastfed infants but we don’t document it. The infant formula is mainly sourced through donations and thus we only distribute when we receive supplies. We recognize that we should only distribute when we have adequate and sustainable pipeline but the current context doesn’t guarantee that. Currently there is a shortage of available formula milk and external aid agencies with experience in supplying infant feeds are also absent yet the numbers of non-breastfed infants and orphans are increasing.” An aid worker, Syria
In Iraq, an already serious humanitarian crisis is growing worse with hundreds of thousands of men, women and children fleeing their homes in the wake of escalating conflict. Recent reports indicate that caregivers are requesting that infant formula be part of baby kits as happened during the national oil for food programme in the mid1990s14.
 Lessons drawn from the ongoing Syrian crisis IYCF-E response
Lessons drawn from the ongoing Syrian crisis IYCF-E response
Although significant gains have been made in the development of IYCF-E policies, initiatives and training materials, we are not there yet. Recurring challenges in translating the policies into practice suggest the need to revisit the current guidelines in establishing a way forward. Although breastfeeding remains one of the most scientifically researched topics, a universal model of determinants of breastfeeding that applies to every country is yet to be developed.
Although some national level gains were made during past emergencies in Iraq and Lebanon (e.g. adoption and endorsement of the Operational Guidance on IYCF-E), the momentum was lost at the end of the crises. In Lebanon, the national policies that were developed and adopted were not translated into practice. For example, despite the adoption and revitalisation of the BFHI during the crisis, the BMS industry remains rife in Lebanon today with health professionals being strong advocates:
“When I delivered a month ago, I had to fight to be allowed to breastfeed my baby. Immediately after delivery, my baby was taken to the nursery and kept away from me. Being a nutritionist, I requested to have my baby close to me. After delivery, I was brought a tin of formula milk with a note from the paediatrician saying it’s good for my baby. When I declined to give my baby the formula milk, I was given a declaration form to sign. The declaration form was clearly supporting formula feeding and citing my refusal to formula feed.” A nutritionist and humanitarian worker, Lebanon
Support for IYCF-E is still regarded as solely a nutrition/health issue while in reality, it is cross-sectoral and can be supported through shelter programmes, food security sectors and protection sectors. Furthermore, limited political will to support IYCF programmes through legislation and adoption of national IYCF policies and guidelines, such as the Baby Friendly Hospital Initiative (BFHI) and the Code, hinders implementation.
“Infant formula is a serious political issue within the Middle East region. I will therefore advise that we approach the issue with a lot of caution.” A government official
The lack of policies, support and an enabling environment for IYCF makes it difficult to implement IYCF support during emergencies. In the ongoing crisis, some international NGO’s have established parallel systems to provide IYCF support to affected populations, which are generally not sustainable post emergency and thus gains are often lost. Furthermore, some field personnel have shown limited ability to establish and provide successful models of IYCF services. There is limited documentation of what works or not which hinders development of models and references.
Although agencies normally review their IYCF-E policies, funding policies and programming responses during crisis, past crisis, particularly Lebanon and Iraq, suggest the momentum is lost after the emergency ends. The experiences and lessons learnt during the Lebanon crisis triggered a review and update of the Operational Guidance on IYCF-E at the global level, yet today Lebanon still has no emergency preparedness plan on IYCF-E. Furthermore, nutrition policies and guidelines that were developed after the crisis ended are yet to be reviewed and implemented. This raises the question, how can we ensure that the gains made during emergencies are sustained and embedded into existing national policies? Besides, in the current Syrian context where artificial feeding was established pre-crisis, should a policy aimed at guiding aid workers and agencies about how to source, distribute and handle infant formula milk within the Syria response be considered? The policy should ensure that sourcing, distribution and handling of infant formula is done in line with international standards whilst maintaining a flexible and pragmatic approach in accordance with the developing security situation in Syria and across Middle East region.
Emergencies can happen anywhere, and humanitarian response plans must be flexible, while still following guidelines. This is especially the case with regard to IYCF, where agencies need to respond to the local context. Agencies must also be aware that addressing IYCF is important in all emergency settings, including middle-income countries, and has inter-sectoral implications. Since emergencies happen fast and unexpectedly, NGOs and staff from all sectors should ensure that IYCF-E policies are in place, and that IYCF-E is included in staff training and materials so that programming is swift and of the highest quality, and that infants and young children are protected.
For more information, contact Suzanne Mboya, email: suzannemboya@outlook.com
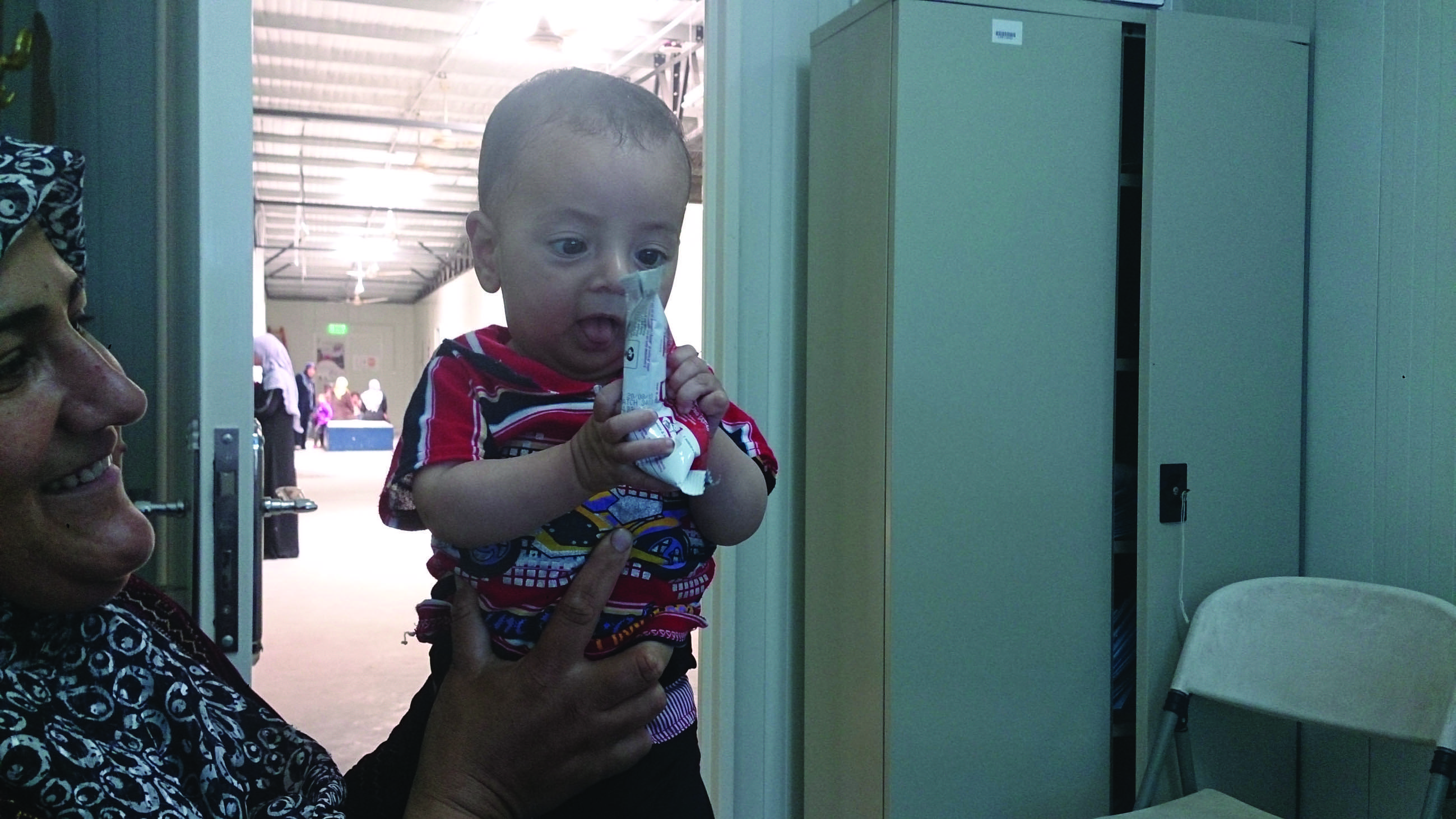 CASE STUDY ONE
CASE STUDY ONE
Jordan: The experience of a young mother who fled the ongoing conflict in Syria
Noor is a first time mother with a five month old daughter-Leila living in Za’atari camp, Jordan for two years. She has been attending baby friendly spaces by Save the Children Jordan since she arrived in Za’atari camp. “I didn’t have much to do at our family caravan so I always accompanied my neighbour, Lizah to the baby friendly spaces. The caravan provides a relaxing atmosphere and allows women to meet and share experiences.” Noor decided prior to delivery that she would practice exclusive breastfeeding having attended many sessions on breastfeeding and infant feeding practices. Although she had hoped to deliver naturally, complications during labour compelled her to undergo a caesarean section making her unable to initiate breastfeeding immediately, as it took long for the anaesthesia to wear off. When she regained consciousness, her baby was already receiving infant formula. When she tried breastfeeding, her baby refused the breast and for ten days, her baby did not breastfeed. “I fed Israh sugar water, herbal- chamomile tea and powdered milk. My breasts were very painful and swollen because Israh was not feeding. I was stressed because I knew the benefits of breastfeeding”. On the 11th day after delivery, Noor was visited by an IYCF counsellor who counselled her about the possible reasons for baby’s refusal to breastfeed.
After three hours of trying to breastfeed with the assistance of the IYCF counsellor, she was able to breastfeed. “I was really happy. After eleven days of agony, Leila was able to latch on and suckle the breast. My nipples were painful and sore but I was happy to finally position and try breastfeeding. The milk did not flow immediately; the right breast flowed first after three days of trying while the left breast flowed after four days.” Noor was pleased by the kind of breast feeding support she received. “The IYCF counsellor really helped me, she sat with me every day and assisted me with breastfeeding and even after the milk came in, she continued to visit me and support me. I am still breastfeeding Leila exclusively” Noor is looking forward to giving Leila complementary foods when she soon turns six months old. Leila is a healthy baby girl who rarely gets sick.
 CASE STUDY TWO
CASE STUDY TWO
Jordan: The experience of a multi-para mother who fled the ongoing conflict in Syria
Basma is a mother of five children. Basma arrived in the heat and dust of Za’atari refugee camp in December 2012 after fleeing the ongoing conflict in Syria. “There was bombing and explosions everywhere. I decided to flee when a bomb fell near our house”. She was exhausted and hungry after travelling for two days with her children. Basma’s husband followed five months later. Basma has practiced artificial feeding with all her children. She was advised to do so by doctors back in Syria after she lost her first two children. “After losing my first two children, I was told my breastmilk was poisonous and should give infant formula instead”. Basma’s older children were often sick and very irritable. “I was always in and out of hospital because of constant diarrhoea.” After learning about safe artificial feeding practices following interaction with IYCF counsellors, Basma has changed the way she feeds her last baby, now four months old and in good health.
“With this child I can sleep well because she is not sick” she said. “I give her only infant formula. I prepare her milk using the preparation instructions given to me by the IYCF counsellors; I prepare small quantities enough for single feeds. I have to maintain hygiene and safely prepare the milk to prevent contamination.” Basma receives infant formula every two weeks from UNHCR through the Jordanian Health Aid Society (JHAS). She recalls that during the earlier days in the Za’atari camp, infant formula was provided by agencies, particularly in field hospitals, to all mothers.
This feeding experience is a sharp contrast to Basma’s previous experience with motherhood when she fed her baby infant formula, sugar water, herbal drinks and sometimes cow milk or yoghurt. “I often took my children to the health centre with abdominal cramping, diarrhoea and vomiting. I would lose money paying the health centre. I used to buy the infant formula from supermarkets and pharmacies back home. It was very expensive so I sometimes used other milks” she recalls. She was not given any information regarding preparation and safe artificial feeding by the hospital staff back in Syria.
Basma is happy with the key messages and support she has received on safe artificial feeding. The key messages she recalled included: need for exclusive formula feeding; preparation procedures-quantity of water and milk to be used; amount to be prepared according to age; hygienic preparation and safe storage of infant formula.
CASE STUDY THREE
Turkey: Experience of a mother of a non- breastfed infant who fled the ongoing conflict in Syria
Sawsan is a mother with three children living in a refugee camp in Nizip, Turkey. Sawsan’s last born Wael, who is now 2 years old, was born in Syria. On the onset of the crisis, after her neighbour’s house was bombed, Sawsan came with her three children and her husband followed later. Sawsan and her family arrived in the dust and heat of after two exhausting days. “Wael was six months old when we arrived in Nizip. Since birth, I have always given Wael infant formula. In Syria, infant formula was easily accessible and available from pharmacies and supermarkets. When the bombs went off, I left my home with only one tin of Nido powdered milk. I prepared this milk for Wael during the journey”. Liza and her older children ate bread and water. Unfortunately her fortunes turned worse at the entry point when someone stole the Nido tin of milk when she was attending to her other children. “At the border, Wael’s tin of milk was stolen and I was left with nothing. I was really stressed and had nothing to give Wael. I gave him water that was given to us at the resting areas at the borders and it really broke my heart.”
Upon arrival at the refugee camp, Sawsan thought she would receive a can of infant formula to give to Wael. However upon examination by the midwife, she was told she did not qualify for the infant formula since Wael was already six months old. She was instead advised to start complementary feeding. “I felt angry and frustrated. How could they deny me the infant formula after everything I had gone through? I felt like the midwife was not really supporting me. However, after two hours of yelling, the midwife finally gave me the formula. I understand that complementary foods should be introduced at six months; the security situation back home did not allow me to do that. I believe the midwife should have given me formula and allowed me to wean Wael gradually. I had to buy formula to give Wael as I gradually gave him the recommended complementary foods. Wael is two years and healthy now; that puts a smile on my face.”
CASE STUDY FOUR
Syria: The experience of an internally displaced mother living in Syria
Zainab is a mother of five children living in Idleb, Syria. After a bomb explosion in which she lost some of her relatives, she took in three children whom she cares for. “I was in the house when the bombs went off. After the chaos, the blast and the commotion died down. The aftermath was beyond comprehension. Yes, I and my children were safe; I just couldn’t say the same for my two sisters and brother in-law. I had lost three relatives in the explosion. I had to take care of three children-Ahmad, Amira and Rasha who had lost their mothers. Ahmad and Rasha were four and five months respectively. It was a very difficult time for me and my family.”
“My last born, Ammar was 4 years old then. When Amar was young, I breastfed him though I sometimes gave him formula milk. The doctor told me to use formula because Ammar used to cry a lot. My breastmilk was not enough. Infant formula was easily available and accessible from the pharmacies. However since the start of the crisis, things have really changed. When I took in Ahmad and Rasha, I was not really prepared on how I would feed them.” Zainab faced a difficult challenge providing for her new adopted children with the ongoing crisis. “Although I received counselling on the possibility of re-lactation, I was not able to try it. Getting infant formula was really difficult. Sometimes I would find and sometimes not. I had to complement with tea, sugar water and any available milk.” The prolonged duration of the Syrian conflict is leading to a widespread shortage of commercially available powdered infant, particularly in opposition-held areas. In addition, any available infant formula is very costly, making it prohibitively expensive for many people.
Zainab introduced complementary foods at seven months. She was faced with further difficulty in obtaining nutritious complementary foods due to market shortages. “I am honestly glad Ahmad and Rasha are above one year old now. They are now eating family foods. It’s still not easy getting food sometimes but it’s much better than searching for infant formula. It sure has been a roller coaster but I am grateful to Allah for his beneficence”.
CASE STUDY FIVE
Jordan: The experience of a first time Syrian mother in Jordan
Nazreen, a first time mother of one month old Heeba recently moved to Za’atari camp from Amman. Nazreen arrived in Amman 21 months ago after 4 long exhausting days. “I fled Syria alone in the heat of the conflict and went to Amman to work as a nanny for a family. I stayed with family for six months then moved to Za’atari camp because the family left Jordan. Back home, I lived with my sister after we lost our parents. I fled leaving my only sister behind.”
Arriving in Za’atari camp, she felt depressed having no one to turn to. She therefore decided to get married to escape loneliness. “I was very lonely and depressed. I married my first husband but things changed after afew weeks. My husband would really beat me up and verbally abuse even when I was pregnant. When I was 7 months pregnant, he beat me up and experiencing intense bleeding, I had to be taken to hospital. I was put on drugs but had to deliver Heeba preterm.”
“After delivery, I divorced my first husband and met my current husband two months later. I experienced complications at birth and had to be separated from Heeba. In addition, Heeba refused to breastfeed and so I gave her dates soaked in water and infant formula. On my discharge date, I met Israh, an IYCF counsellor at the protection centre after referral by UNHCR. Israh was very good to me. She advised me on the importance of breastfeeding and offered breastfeeding support with positioning and latching. After three hours, Heeba was able to latch onto my breast and start suckling. I was also given a breast pump to help with expressing milk. After three days, milk begun to flow. I am currently breastfeeding Heeba exclusively.”
Living alone with no family support and prior breastfeeding experience, IYCF counsellors provide a lot of IYCF support to Nazreen. She also receives information about childcare practices, immunisation and hygiene. “I am very grateful to Save the Children for their support. The IYCF counsellors visit me on a weekly basis and assist me with my nutrition needs.” Fortunately, her current husband is very supportive and caring for both her and Heeba.
1 Syrian Crisis IYCF-E end of mission report, 31st August, 2014
2 MOH, nutrition surveillance system report 2011
3 MOH, 1998
4 MOH, 2006
5 Rapid Nutrition Assessment report in Northern Syria; Emma Littledike for Nutrition sub-working group 9/3/2014
6 Desk review of nutrition rapid assessment reports compiled by Nutrition Working Group; Turkey, May 2014
7 HIHS Policy on the use and distribution of powdered infant formula milk, 2014
8 Experiences and Reports by INGOs and NGOs responding in Syria
9 According to the Code, a breastmilk substitute is any food being marketed or otherwise represented as a partial or total replacement for breastmilk, whether or not suitable for that purpose. These include infant formula, other milk products, therapeutic milk, and bottle-fed complementary foods marketed for children up to 2 years of age and complementary foods, juices, teas marketed for infants under 6 months.
10 Syrian Code of Marketing of Breast-Milk Substitutes, Regulative Resolution Number 19/T Date 03/07/2000
11 See the article by MSF on the subject of acute malnutrition in infants under 6 month of age in Northern Syria in this edition of Field Exchange.
12Version 2.1 (2007) Available at http://www.ennonline.net/operationalguidanceiycfv2.1
13Infant Formula Distribution in Northern Iraq. Field Exchange 20, November 2003. p5. www.ennonline.net/fex/20/infant
14 This is dried milk powder and is not an infant formula

