Treatment of malnutrition in Lebanon: Institutionalisation with the Ministry of Public Health – steps and lessons learned
By Linda Shaker-Berbari, Pressila Derjany Khoueiry and Dima Ousta
 Linda Shaker Berbari works with International Orthodox Christian Charities (IOCC) as Regional Technical Advisor on Health, Nutrition and Infant and Young Child Feeding (IYCF) for the Middle East region. Between October 2013 and January 2015, she was Country Representative for IOCC Lebanon, overseeing operations in Lebanon. Linda has more than 15 years’ experience in community nutrition, including nutrition in emergencies and IYCF.
Linda Shaker Berbari works with International Orthodox Christian Charities (IOCC) as Regional Technical Advisor on Health, Nutrition and Infant and Young Child Feeding (IYCF) for the Middle East region. Between October 2013 and January 2015, she was Country Representative for IOCC Lebanon, overseeing operations in Lebanon. Linda has more than 15 years’ experience in community nutrition, including nutrition in emergencies and IYCF.
Pressila Derjany Khoueiry is the Health Programme Coordinator at IOCC. Pressila has a BSc in Nutritional Sciences and University Diploma in Human Lactation and Breastfeeding.
Dima Ousta was the Health and Nutrition Programme Coordinator at IOCC between September 2013 and October 2015. Dima worked as a Consultant for UNICEF in Serbia and Greece on IYCF-E in 2015 and 2016 response to the Europe Refugee and Migrant Crisis and and has recently joined Nurture Project International (NPI) as a virtual volunteer for the IYCF-E response in Greece.
The authors wish to thank UNICEF Lebanon for funding and support in Phase 2 and UNHCR Lebanon, the primary funder for Phase I, for their continuous support. Thanks also to the Ministry of Public Health in Lebanon, the staff of its network of Primary Health Care Centres (PHCs), and the Ministry of Social Affairs in Lebanon and its Social Development Centres. A word of appreciation for the hard work and dedication of all of IOCC staff and to Pierre Felefli for the Training of Trainers. Special thanks to the American University of Beirut, especially to Dr. Hala Ghattas and Dr. Omar Obeid for their continuous technical support. Finally, the authors gratefully acknowledge the support of Farah Asfahani and Elsie Abou Diwan in reviewing this article.
Location: Lebanon
What we know: Between 2011 and 2014, services to treat acute malnutrition among Syrian refugees in Lebanon were scaled up and delivered by IOCC at primary health centre (PHC) level.
What this article adds: From 2015, acute malnutrition treatment services were transitioned to integrate within PHCs, led by the Ministry of Public Health (MoPH) in close collaboration with UNICEF. PHC staff were tasked with screening, referral and treatment as routine activity. IOCC’s role transitioned from direct implementation to resource review and update, training (workshops and on-the-job), and mentoring (two three-month periods of support, 2015 and 2016). A significant challenge to integration is competing demands on health workers that limit/preclude screening and treatment, with calls for incentives/more staff (neither are provided). Ongoing training of staff is needed at facility level to refresh staff knowledge and allow for turnover when needed. Therapeutic foods are currently provided by UNICEF to PHCs; subsidised consultation costs are met by families. The leadership and management of MoPH is essential to sustainability; quality assurance of staff and services informed by collation of caseload data and outcomes of treatment is needed.
Background
International Orthodox Christian Charities (IOCC) started its nutrition programme in Lebanon as a result of the Syrian refugee crisis. From 2011-2014, the number of refugees increased and cases of acute malnutrition started to appear. In response, IOCC, with support from UNICEF and UNHCR, initiated malnutrition treatment in primary health care centres (PHCs) in the form of community-based management of acute malnutrition (CMAM) and contributed to capacity-building of the Lebanese Ministry of Public Health (MoPH). This programme was implemented in selected vulnerable localities in all six governorates of Lebanon and described in a 2015 article in Field Exchange (Berbari et al, 2015).
This article continues the story of the work by IOCC during and after 2015. It describes programme phase-out and transition of acute malnutrition treatment services to the public health services in Lebanon, aiming to institutionalise them. This was achieved through a preparation and implementation phase involving co-review of programme materials and forms with the MoPH and UNICEF, recruitment of nutrition mentors and internal training of trainers (TOT), training rollout, and coaching, mentoring and monitoring of implementation.
Introduction
During phase 1 of the programme (ibid), IOCC screened 60,000 children under five years of age for acute malnutrition; 2,400 cases were identified and treated. Forty-two PHCs were engaged in the screening and treatment of malnutrition through support from IOCC human resources. Starting at the end of 2015, the MoPH conducted a cost-benefit analysis of the nutrition programmes in Lebanon. Based on this and available data on the nutritional status of children, it developed a recommended integration of activities within its network of PHCs to enable sustainability of activities and preparedness of centres to respond.
IOCC’s role accordingly changed drastically from frontline, direct contact with beneficiaries to trainer and mentor for the implementation of an integrated programme. Activities were revised and implemented as per MoPH recommendations. A new programme was developed – Phase 2 – focused on capacity-building and provision of on-the-job support (mentoring) for PHCs within the MoPH network, alongside other non-governmental organisations (NGOs), Relief International and AVSI (www.avsi.org). The programme also involved support to PHCs to report on the nutrition indicators of all children under five years old as part of the Health Information System (HIS), training of mobile team staff of a local NGO on screening and referral of acute malnutrition at the field level, and training a selected number of Ministry of Social Affairs (MOSA) Social Development Centres (SDCs) on screening and referral of acute malnutrition.
In terms of nutritional status, global acute malnutrition prevalence was low (4.5%, SMART surveys, 2012, and 2.2% in the most recent SMART survey of 2013 (UNICEF, 2014). Anthropometric results of refugee children 0-59 months from the 2016 Vulnerability Assessment of Syrian Refugees (VASyr) data show a GAM rate of 2.3%, which indicates stability throughout the years.
However, the latest 2016 VASyr (WFP, UNHCR, UNICEF, 2016) also reveals significant causes for nutrition concern; in particular, a high disease burden among children under five years old and inappropriate infant and young child feeding (IYCF) practices. While there was a small increase in exclusive breastfeeding (EBF) rate compared with 2015, only 3% of children aged 6-23 months met the minimum acceptable diet; 15% of children aged 6-17 months met the WHO recommended minimum diet diversity thresholds; and 18% of children aged 6-23 months met the WHO recommended acceptable meal frequency. Also, only 62% of children aged 6-23 months were found to consume solid foods.
Until 2015, the cost of treatment of malnutrition, including transportation of families to and from the PHC, was supported by UNICEF, UNHCR and other NGOs. Programme supplies including ready-to-use supplementary food (RUSF) and ready-to-use therapeutic food (RUTF) were provided by UNICEF and distributed through IOCC. UNICEF and MoPH jointly covered the cost of treatment in Phase 2. Supplies were provided to PHCs by UNICEF and provided free to families. A subsidised cost for the medical consultation was paid by the families; Syrian refugees get further subsidised costs from supporting NGOs. In Phase 2, programme data on caseload and nutritional status of children attending PHCs was sent directly to the MoPH by the PHCs, rather than being compiled by IOCC.
Preparation for Phase 2 took place between July and August 2015. It included co-review of all programme materials and internal capacity-building of IOCC to deliver trainings and launch the mentorship programme in 2015. In 2016 a second round of training and mentoring took place, based on the needs identified and requested by MoPH and UNICEF.
Preparation
Review of training and programme material (July-August, 2015)
The development of resource material for screening and management of malnutrition devised in Arabic was an important output of the overall project. This included training materials, treatment forms and referral forms for outpatient and inpatient management of both moderate and severe acute malnutrition (MAM and SAM).
As Lebanon does not have a national protocol for the treatment of malnutrition, the programme drew on international guidelines such as the Harmonised Training Package (HTP)1 and WHO updated guidelines on management of SAM2. The programme also relied on experts from the American University of Beirut, who were engaged in the Regional Nutrition in Emergencies Training to adapt the material. At the same time, MoPH with UNICEF have built on the resulting material to develop a national protocol; this has not yet been formalised.
Training material used during Phase 1 was extensively reviewed and approved by MoPH in 2015. In 2016, the same materials were used, with an additional section on nutrition screening and treatment of pregnant and lactating women. Training content is overviewed in Box 1. Two healthcare staff nominated by each MoPH network PHC and selected SDCs attended a two-day training on screening and referral of acute malnutrition. PHCs selected by MoPH to become treatment centres received an additional one-day, facility-based training on the outpatient management of MAM and SAM and referral for inpatient treatment.
Box 1: Overview of training content
Training on screening and referral of acute malnutrition, two days
Day 1:
- Introduction to Nutrition in Emergencies and the importance of preparedness in Lebanon.
- Basics of infant and young child feeding, the International Code of Marketing of Breast-milk Substitutes, Law 47/2008 in Lebanon, and distribution of existing information, education and communication (IEC) materials.
- Anthropometric measurements of acute malnutrition for children under five years of age (theoretical session).
- Use of growth charts.
Day 2:
- Anthropometric measurements of acute malnutrition for children under five years of age (practical session with live simulation exercises)
- Micronutrient supplementation.
- Reporting and use of programme forms.
- Reporting on the HIS (session was covered by MoPH staff).
- Case studies.
Additional parts for one-day, facility-based training on management of acute malnutrition:
- Management of MAM and SAM for children under five years of age.
- Management of acute malnutrition for PLW (added in 2016).
Training on community screening and referral of acute malnutrition – one day
- Introduction to Nutrition in Emergencies and the importance of preparedness in Lebanon.
- Anthropometric measurements of acute malnutrition for children under five years of age (theoretical session and simulation).
- Use of programme forms (referral forms).
- Basics of infant and young child feeding.
Recruitment of mentors and training of trainers (August-October 2015)
To ensure quality interventions and enable simultaneous, standardised trainings across the different regions in Lebanon, an internal, six-day training of trainers (TOT) was organised in 2015 for the IOCC Health and Nutrition team. For the second round of training and mentoring, in 2016 a two-day internal refresher TOT was conducted. The main TOT covered training skills (adult and peer education, development of lesson plans, interactive training skills, etc) and the lesson plans for each of the sessions of the two-day and facility-based trainings.
In parallel, preparations for the mentoring phase were underway, ranging from finalisation of forms, monitoring and reporting tools to the recruitment of 20 nutrition mentors. IOCC built on existing programme forms and tools that were reviewed and approved by the MoPH; reworked forms were developed in close collaboration with MoPH and UNICEF. IOCC’s programme structure and teams were rearranged to accommodate the change from frontline to mentoring role. Recruitment focused on individuals with a nutrition background and CMAM experience from previous programmes in Lebanon (implemented by IOCC, Relief International or Action Against Hunger). All those recruited attended a one-day internal training on mentoring skills and received guidance on the different mentoring cycles and possible scenarios. The aim of this training was to standardise the coaching approach in all PHCs across Lebanon and deliver the same on-the-job support to all staff involved in the integration of CMAM services in the PHCs.
Implementation
Capacity-building and training of all MoPH PHCs (August-October 2015)
As described above, a series of capacity-building trainings (workshops) took place over two periods; August to September 2015, and August to September 2016. Key training activities delivered were:
- In 2015, two-day training on malnutrition screening and referral of children under five years old across all areas in Lebanon for 217 MoPH PHCs. In 2016, these were condensed to one-day refresher training – on guidance from the MoPH – and were conducted for 214 MoPH PHCs.
- A total of 427 healthcare providers (nurses, physicians and midwives) attended the training in 2015; 269 attended in 2016.
- A one-day, facility-based training on treatment of acute malnutrition for children under five years old was delivered on-site to 63 PHCs in 2015 and 62 PHCs in 2016.
- In 2016, a one-day training on screening and referral of acute malnutrition was delivered to 85 SDCs under MOSA (90 healthcare providers attended).
- In both 2015 and 2016, IOCC trained field teams from BEYOND, a local NGO, on community screening for malnutrition, both in the North and in the Bekaa Valley. A total of 51 and 101 health staff attended the training in 2015 and 2016 respectively.
Coaching and mentoring of PHC staff (October-December 2015 and October 2016-December 2016)
A key component of the programme was the provision of on-the-job coaching and mentoring in 161 PHCs for screening and referral and for screening and management of acute malnutrition in 41 PHCs. In 2015, IOCC provided mentoring to 204 PHCs, AVSI to 10 PHCs in the South, and RI to 11 PHCs (three in Beirut/Mount Lebanon, two in the North and six in the Bekaa Valley), covering a total of 225 PHCs. Mentors from RI and AVSI had attended the trainings of the respective PHCs that they were scheduled to mentor.
The aim of this activity was to provide support for existing staff to carry out new tasks related to screening and treatment of malnutrition and to support reporting on nutrition indicators. All PHC staff who had attended the MoPH training received facility-based, refresher training as the coaching started. One mentor/coach was present at the PHC periodically or as needed. Each nutrition mentor reported back to his/her respective area coordinator. The scope of work of the mentor is described in Box 2.
At the end of the three-month mentoring period, each nutrition mentor completed a narrative report for each PHC, including PHC background information, summary of visits, challenges, solutions, positive initiatives and recommendations. Each report completed with an interview swith the PHC director and nurse involved in screening, in order to feedback regarding the integration of services.
On recommendation from MOPH and UNICEF, and given the observed need to provide further support for PHCs, IOCC launched a second stage of mentoring in 2016. Field teams were recruited using the same approach as in 2015. A total of 223 PHCs (62 treatment and 161 screening centres) were supported.
Box 2: Nutrition mentor activities
Each mentor covers 10 to 12 PHCs, visiting each PHC once a week or biweekly, as required. The nutrition mentor meets the PHC Director and all PHC staff, explains the details of the CMAM programme, and coaches relevant staff on malnutrition screening and referral. The nutrition mentor engages in screening activities to demonstrate the procedure. In management centres, the nutrition mentor meets with paediatricians to follow up on the treatment of acute malnutrition. On each visit, the nutrition mentor fills out a daily checklist with criteria on programme activities to evaluate the quality of the work within each PHC. On-the-job training is also provided as needed.
Each nutrition mentor sends out an advance weekly schedule detailing planned visits and activities, and submits an end-of-week output report, including quantitative and qualitative data about each centre visited.
Some centres showed positive engagement and initiatives in organising IYCF-awareness sessions at the PHC and the nutrition mentor was always readily available to assist in delivering related information. IEC materials distributed during the trainings were used as reference.
Challenges and lessons learned
Implementation and sustainability of nutrition activities at the PHC level
A number of challenges and lessons learned were highlighted on the sustainability of such activities within PHCs. These included:
The support and endorsement of MoPH is essential for the successful implementation of planned activities by PHCs and compliance with training requirements.
Regular training on screening, referral and/or management of acute malnutrition is necessary as refreshers to trained staff and to provide the opportunity for more staff from PHCs to be trained. This becomes especially important given staff turnover in PHCs. Those trained were not always the ones in charge of implementing the programme at the PHC level; mentors had to provide on-the-job training as needed in order to equip the right staff with the necessary skills. Between the first phase and the second phase of training, a number of staff had changed; therefore, for many, the training delivered by the mentor was their first.
It is important to consider the long-term consequences of providing incentives to healthcare staff for screening and management of acute malnutrition. Providing monthly incentives to PHC staff to take measurements will certainly ensure better staff compliance and motivation, yet incentives may also act as a challenge to sustainability as soon as they can no longer be provided (i.e. when funding is no longer available). Feedback from participants in the training highlighted the need for additional staff in PHCs in order to accommodate and run nutrition activities in a smooth manner. Throughout the mentoring phase, the MoPH decided that incentives would not be paid to PHC staff involved in malnutrition management and that PHCs should provide these services as part of their daily tasks and activities. Thus, provisions must be made within the MOPH’s strategy to ensure a proper human resource structure is in place and that capacity is adequate to run programmes related to child growth.
Reporting and information management is challenging for PHCs who have a limited number of staff and/or who use both written and computerised reporting, as this may create errors. Tablets linked to the HIS have been proposed to be used directly at screening as they are user-friendly and there is less room for error.
Challenges related to the integration of malnutrition services in the PHCs
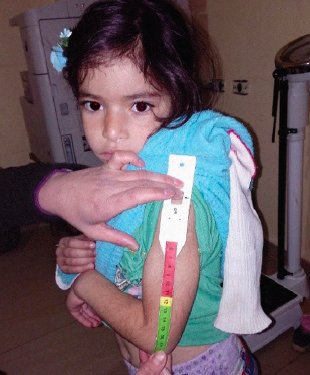 IOCC staff faced challenges in both mentoring phases. During mentoring visits, PHC staff were constantly overloaded with other PHC activities and barely had time for refresher trainings or for actual screening activities, or even demonstration of screening. With perseverance, nutrition mentors were able to convince the staff of the importance of screening, and this resulted in allocating time daily for malnutrition screening. However, this did not work in all PHCs, as shown in the narrative reports submitted to the MoPH and UNICEF. Many of the PHCs still do not actively screen for malnutrition or only screen when the nutrition mentor is present. As noted above, PHC staff were asking for additional staff to be hired to assist with daily duties, as well as incentives to motivate existing staff involved in malnutrition screening.
IOCC staff faced challenges in both mentoring phases. During mentoring visits, PHC staff were constantly overloaded with other PHC activities and barely had time for refresher trainings or for actual screening activities, or even demonstration of screening. With perseverance, nutrition mentors were able to convince the staff of the importance of screening, and this resulted in allocating time daily for malnutrition screening. However, this did not work in all PHCs, as shown in the narrative reports submitted to the MoPH and UNICEF. Many of the PHCs still do not actively screen for malnutrition or only screen when the nutrition mentor is present. As noted above, PHC staff were asking for additional staff to be hired to assist with daily duties, as well as incentives to motivate existing staff involved in malnutrition screening.
Some PHCs were quite remote and at times reaching them was challenging for beneficiaries. These PHCs presented very low caseloads of paediatric patients and reported zero cases of screened children monthly.
After the first mentoring phase, the majority of the PHCs did not carry on with the project activities; PHC staff restarted the screening process when the second mentoring phase began.
So far, implementation has been driven by the availability of ad hoc funding; there is no clear plan regarding steps for a complete phase-out of external support for the activities.
Lack of transportation payments for families and financial coverage of inpatient treatment for cases with complicated SAM were a common challenge to proper case management. MoPH needs to budget for these additional costs when planning for a sustainable integration of malnutrition services in the PHCs.
Recommendations
Recommendations to ensure sustainability of the integration of nutrition services at the PHCs include the following:
PHC staff should be mandated by MoPH to provide malnutrition screening and treatment services. MoPH engagement in routine monitoring and evaluation of PHC staff performance is a priority to assess whether implementation of programme activities is on track and to ensure successful programme continuity. Regular refresher training on screening and management are needed to ensure all relevant staff are trained and updated. Exchange visits of PHC staff conducting screening/treatment with staff in management PHCs should be promoted to allow all to experience the comprehensive programme.
Strong endorsement of PHC-level malnutrition activities by MoPH should be ensured by increasing the number of MoPH staff responsible for supervising activities at PHCs. The latter need to be trained on acute malnutrition in all its components, allowing them to become a reference and provide sustainable support for PHC staff.
The MoPH should analyse the data compiled from the HIS to inform on the nutritional status of children in Lebanon and caseload across PHCs and regions on the management of MAM and SAM.
IYCF services should be incorporated into the primary healthcare system, which requires capacity-building of health workers to implement IYCF counselling and support, incorporation of IYCF services into maternal and child health, and strengthened links and referrals with inpatient and outpatient acute malnutrition treatment services.
For more information, contact: Linda Shaker-Berbari, email: lberbari@iocc.org
1 GNC, ENN and NutritionWorks (2014). Harmonised Training Package (HTP) version 2. www.ennonline.net/resources/htpversion2df
2 WHO (2013). Updates on the Management of Severe Acute Malnutrition in Infants and Children. apps.who.int/iris/bitstream/10665/95584/1/9789241506328_eng.pdf
References
Linda Shaker-Berbari, Dima Ousta and Farah Asfahani (2015). Institutionalising acute malnutrition treatment in Lebanon. Field Exchange 48, November 2014. p17. www.ennonline.net/fex/48/institutionalising
UNICEF, 2014. 2013 Joint Nutrition Assessment Syrian Refugees in Lebanon. www.unicef.org/lebanon/resources_9771.html
WFP, UNHCR, UNICEF, 2016. Vulnerability Assessment of Syrian Refugees in Lebanon 2016. documents.wfp.org/stellent/groups/public/documents/ena/wfp289533.pdf


