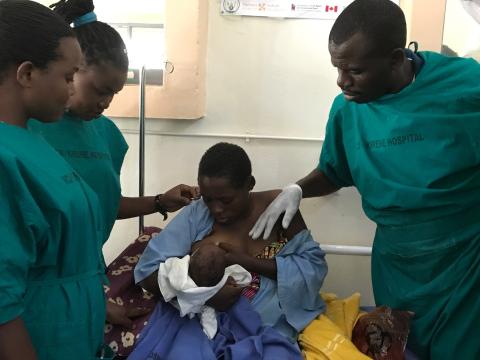
Improving practical skills for breastfeeding vulnerable infants in low-resource settings: training material development and a case study from Rwanda
Read a summary of this field article here.
By Himali de Silva and Maya Asir with contributions from Kathryn Beck, Catherine M Kirk, Gato Saidath, Marie Louise Manirakiza and Egide Karangwa
Himali de Silva is a speech and language therapist working for the National Health Service (NHS) in the UK, where she works as a clinical specialist in infant feeding. She has worked in several countries, including Sri Lanka, Cambodia, Russia, Malawi, Rwanda and Uganda, providing training to healthcare professionals in managing paediatric feeding disorders.
Maya Asir is a speech and language therapist working for the NHS in the UK, where she works as a clinical specialist in infant feeding in a hospital setting. She has worked in several countries, including Sri Lanka, Malawi, Rwanda and Uganda, providing training to health professionals in managing infant feeding disorders.
Kathryn Beck is the Senior Nutrition Program Manager at Partners In Health/Inshuti Mu Buzima, Rwanda. She is a registered dietitian with over seven years’ experience of clinical nutrition practice and four years’ experience working internationally on paediatric nutrition programming.
Catherine M Kirk is the Director of Maternal and Child Health at Partners In Health/Inshuti Mu Buzima, Rwanda. She has over seven years’ experience in child health programming and evaluation, with a specific focus on health-system interventions to promote neonatal survival and optimal early childhood development.
Gato Saidath is a Maternal and Child Health Program Officer at Partners In Health/Inshuti Mu Buzima, Rwanda. She is a registered midwife with over eight years’ experience in clinical practice in maternity and more than two years’ experience in providing clinical trainings and mentorship.
Marie Louise Manirakiza is a registered nurse who worked for two years as an All Babies Count Quality Improvement Advisor at Nemba District Hospital before being promoted to Mental Health Program Manager at Partners In Health/Inshuti Mu Buzima, Rwanda.
Egide Karangwa is a Maternal and Child Health Program Officer at Partners In Health/Inshuti Mu Buzima, Rwanda. He is a registered midwife with over eight years’ experience in clinical practice, as well as in leadership, training and mentoring.
The authors would like to thank the contribution of Rwinkwavu District Hospital and Kirehe District Hospital neonatal, maternity and post-partum clinicians and staff, as well as advisors, researchers and data analysts who contributed to this work and the day-to-day operation of the hospital units. We would also like to thank the patients and caregivers for entrusting us and the entire team with their healthcare and the Ministry of Health Rwanda, who operates the district hospitals. We would also like to thank Multi Agency Training and Support (MAITS) for publication of the Working with Infants with Feeding Difficulties (WIFD) training programme and their logistical support of the trainers, and The Primate’s World Relief and Development Fund (PWRDF) through Global Affairs Canada and The Funding Network, who funded the training in Rwanda.
Location: Rwanda
What we know: Premature infants and those requiring intensive neonatal care have significant feeding difficulties that require specialist support.
What this article adds: The Working with Infants with Feeding Difficulties (WIFD) training package was developed by Multi Agency International Training and Support (MAITS) to address a gap in training content on feeding issues of vulnerable infants for frontline healthcare staff of neonatal intensive care and special-care baby units in low resource settings. The package comprises classroom and practical work and training of trainers. WIFD has been trialed in Malawi, Uganda, Sri Lanka and Rwanda in nine hospitals, involving 175 healthcare staff. In Rwanda (2018), for example, pre- and post-test evaluations among 21 trainees found a rise in trainees’ test scores (54% v 90%) and in self-reported confidence, knowledge and practical skills (67% medium and 28% low v 95% high). Pre- and post-training comparisons found significant (p<0.001) improvements in breastfeeding on day of birth (11.3% to 26.9%)); delayed introduction of breast milk (49.6% to 36.2%); and exclusive breastfeeding at discharge (63.1% to 75.9%). Master Trainers have trained 70 health providers across 10 hospitals, two more Master Trainers and ‘Expert Mothers’ (to provide peer breastfeeding support to mothers in neonatal units). Opportunities are being explored to integrate this training into existing packages, such as Kangaroo Mother Care, to enable sustainable scale-up.
Background
Establishing and maintaining successful breastfeeding continues to be a global challenge, despite strong evidence to suggest its importance in infant survival. Breastfeeding vulnerable infants in special care and neonatal units in low-resource settings poses further difficulties due to infants’ prematurity and intrapartum-related illnesses. A review of relevant training materials available for frontline staff on breastfeeding high-risk infants revealed a significant gap in targeted training for these care groups, particularly with regard to how to support the infant-mother dyad in these circumstances (Box 1). Another fundamental omission in existing training is addressing the risk of aspiration (i.e., inhaling milk into the lungs during feeding) in these infants (Jadcherla, 2016). Among the group of premature infants and infants with birth asphyxia and congenital anomalies who may appear to be able to feed using generic intervention strategies, there is a significant proportion who are unable to coordinate sucking, swallowing and breathing required for safe feeding. Without specific intervention strategies to minimise this risk, these infants will go on to develop lower respiratory tract infections from aspirated material. Additionally, these infants face long-term nutritional and growth challenges with higher rates of chronic and acute malnutrition (Christian et al, 2013; Kakooz-Mwesige et al, 2015). The heterogeneous nature of these infants poses a challenge when developing a robust training package that meets the needs of at least the majority of high-risk infants. It is essential that training addresses assessment of an infant’s feeding behaviours and skills prior to feeding, especially prior to directing them to cup-feed or feeding with a spoon, syringe or dropper where the feeder is advised to pour the milk directly into the baby’s mouth (WHO, 2003). There is a significant gap in current training materials on identification of specific feeding difficulties and, as such, the interventions offered do not support the feeding development of this group of high-risk infants.
Given this, our aim was to develop a training package to fill these gaps as a complement to currently available training for frontline staff, which could stand alone or be used as an adjunct to other courses, such as the courses identified by the authors in Box 1. This article describes the training approach developed, rollout to date and experiences of implementation in Rwanda in collaboration with Partners in Health (PIH). PIH is an international non-governmental organisation (NGO) that partners with the Rwandan Ministry of Health to develop paediatric development clinics (PDCs) in response to a need for outpatient, long-term clinical, nutritional and developmental follow-up of infants born preterm, with low birth-weight (LBW), or other birth or perinatal complications. While the PDCs were found to address a critical gap in care for vulnerable infants, challenges remained, particularly around early identification and management of breastfeeding difficulties and nutritional outcomes (Beck et al, 2018).
Box 1: Findings of review on training materials for high-risk infants
The World Health Organization (WHO) developed guidelines on optimal feeding of low birth-weight infants (LBW) in low and middle-income countries in 2011 (WHO, 2011). The guidelines cover a range of recommendations, such as when to initiate feeding, what to feed and relevant supplementations; however, there are no recommendations on how to support the infant-mother dyad.
Most breastfeeding-related training materials are aimed at community-based health workers. The WHO/UNICEF 40-hour breastfeeding counselling course (WHO and UNICEF, 1993) and five-day Infant and Young Child Feeding (IYCF) Counselling: An Integrated Course (WHO and UNICEF, 2006) are two such well established courses. The course on Integrated Management of Childhood Illnesses (IMCI) (WHO, 2019) addresses breastfeeding training for staff at first-level health facilities. WHO’s practical guide on Kangaroo Mother Care (KMC) (WHO, 2003), aimed at healthcare professionals supporting preterm infants, covers both breastfeeding and alternative feeding.
The two WHO training programmes aimed specifically at health professionals working with inpatients in neonatal and special care units are Pregnancy Childbirth, Postpartum and Newborn Care (PCPNC) course (WHO, 2006) and the Essential Newborn Care (ENC) course (WHO, 2010). Both courses address feeding-related difficulties in the first day of life or until discharged from hospital. Some guidance is provided on feeding vulnerable infants – if risks are identified, they are directed to one of two management options: (1) “counsel on breastfeeding” with instructions to keep the baby longer at the breast; and (2) initiate “alternative feeding methods”, including hand expression of breastmilk directly into baby’s mouth and cup-feeding.
Training approach
The conceptual model in Figure 1 (Rollins et al, 2016) incorporates the many components of an enabling environment for breastfeeding and highlights the multi-level influences of a successful breastfeeding programme and its rollout. An analysis of health-system bottlenecks for the inpatient care of vulnerable infants in low-resource settings (Moxon and Lawn, 2015) identified “health workforce” as a “very major” or “significant” bottleneck, along with “health financing” and “community participation”. Almost all countries participating in this study identified the lack of trained personnel in neonatal care as a significant bottleneck in terms of quantity and quality of care; one proposed solution for which was the scaling-up of simplified, skills-based training programmes on feeding. Participants specifically highlighted the need for competency-based training and refresher training.
Figure 1: Conceptual model for breastfeeding support (Rollins et al, 2016)

A recent evaluation of essential newborn care (ENC) training in India and Kenya identified key areas for course improvement, including additional time for hands-on practice, practice in a clinical setting and the addition of video learning aids (Thukral et al, 2015). This kind of practical training would help develop high-quality clinical skills, critical thinking, problem solving and would build confidence. This level of investment is likely to ensure engagement from trainees, so that they not only deliver services but also train others in safe feeding practices.
Trainees who experience success first-hand at supporting infant-mother dyads to position and establish breastfeeding are likely to continue using the strategies that helped and support others to do so. Such trainees can become breastfeeding champions who advocate for infants and mothers and promote breastfeeding training in their facilities. These trainees, whose knowledge and skills are strengthened over time, will become local experts. Such a training model would not only be cost-effective but sustainable over time. Formally training trainees to train others would structure the delivery of the material and ensure quality of information passed on.
Working with Infants with Feeding Difficulties (WIFD) training package
WIFD is a training package developed for frontline healthcare staff working in low-resource settings. It specifically addresses feeding-related issues encountered by staff working in neonatal intensive care and special-care baby units (De Silva and Asir, 2017). Focus populations are infants with birth or neonatal risk factors for health and growth failure, including premature infants and infants with neonatal encephalopathies and congenital cranio-facial anomalies. The main focus of the training for these infants is timely identification and intervention in order to prevent deterioration of feeding. The training also benefits infants who have no known previous medical history and have been identified with severe acute malnutrition (SAM), or who have been screened using the PCPNC and identified as not suckling, stopped feeding, presenting with other critical signs such as fast/slow breathing, increased heart rate and no movement, floppy or stiff, and have been referred for hospital-level care. WIFD aims to train staff in the management of these special populations by supplementing interventions relating to counsel on breastfeeding and alternative feeding methods (as defined in the PCPNC) with more specialist management strategies. These strategies promote the establishment of breastfeeding, while ensuring that feeding is safe to reduce feeding-related respiratory illnesses. Although the course is aimed at hospital staff, it is a standalone training programme with flexibility to be adapted to other settings, such as first-level health facilities and community-health settings.
Training of staff
WIFD is currently delivered by two course directors employed by Multi Agency International Training and Support (MAITS), a charity that aims to improve access to healthcare and education for people with disabilities through training. The aim is for trainees of the course to take a lead on training others in the country and region. The training emphasises developing clinical reasoning and problem-solving skills. The package consists of four hours of classroom-based training (more if extra time is needed for translation) and five hours of practical work, usually delivered over two days.
There are five modules in the classroom-based training: lactation, understanding infants with feeding difficulties (identification and assessment, including a breastfeeding checklist), intervention, special populations and case discussions. The training style is interactive and uses a variety of approaches, including presentations, small-group work, video-based problem-solving with prompt questions, clinical reasoning and case analyses. Practical sessions take place in the special care and neonatal units in trainees’ work settings and are structured to mirror the trainees’ developing knowledge and skills. Trainees are supported through guided observations, hands-on training and clinical discussions.
Training of Master Trainers
The package also includes a five-to-six-day training course for future trainers (referred to as Master Trainers). This involves:
- A two-day course attended by two Master Trainers-in training and 10-12 participants;
- A one-day additional mentored practice in specialist care settings attended by the Master Trainers to consolidate clinical skills;
- A one-day period in which Master Trainers prepare to teach WIFD.
- A two-day WIFD course for 12 invited participants organised and taught by Master Trainers; and
- A meeting of Master Trainers and organisational staff at the end of the training to discuss how the course progressed and to prepare for the future.
Master Trainers take significant responsibility from the onset. They familiarise themselves with content of the training, including in the local language, practice giving presentations, facilitate group discussions and lead practical sessions. They work closely with the course directors to gain confidence in independently supporting mother-infant dyads to breastfeed. In addition, once the course is complete, they arrange clinical sessions to practice skills, keep records, video record their sessions and have discussions with other Master Trainers. As part of the training, the course directors offer remote supervision sessions for problem-solving and case discussions. A set of breastfeeding competencies were developed to guide the development of Master Trainers’ clinical skills. Once they start to conduct further training, the Master Trainers then have the added responsibility of guiding and supervising their trainees. Master Trainers are encouraged to take ownership of WIFD training, including its implementation and rollout.
The training package has been trialled in Malawi, Uganda, Sri Lanka and Rwanda across nine hospitals. A total of 175 healthcare staff have received training to date, including three Master Trainers.
Rwanda training: key outcomes
WIFD was delivered in Rwanda to 21 health workers through a partnership between PIH and MAITS in February 2018. The practical sessions of the training were delivered in the neonatal care, post-partum, caesarean section and maternity units of Rwinkwavu District Hospital, a government hospital located in the eastern province of Rwanda. Three Master Trainers were also trained by the course director rather than two, due to the needs of the partner organisation and the advanced skills of the Master Trainer candidates. Both sessions had participants from various backgrounds, including nutritionists, nurses and midwives working at both PIH and across two Ministry of Health (MoH)-supported health facilities. Since the original training, two additional Master Trainers have been trained by the Master Trainers in Rwanda, with remote support from the course directors.
Master Trainers are PIH staff who were chosen based on specific criteria, including clinical skills and knowledge, relevant usual job function (all routinely work with and mentor health workers in MoH-supported health facilities, including hospital neonatal and maternity units), and a desire to share their knowledge and skills with others through additional training and mentoring. Prior to the WIFD in Rwanda, Master Trainers and most participants in the training had received breastfeeding training through the ENC training modules, as well as additional specialised training on the inpatient care of sick and small newborns according to Rwanda’s national protocol, or training on the use of the community management of at-risk mothers and infants (C-MAMI) tool through the PDC. These trainings cover the essentials of breastfeeding and breastfeeding problems (although they are mainly focused on breast problems of the mother and counselling in the case of C-MAMI). Most participants therefore had limited previous training on the identification and management of specific feeding difficulties.
The WIFD trainings were evaluated through a pre/post-test and trainees’ self-reported confidence, knowledge and practical skills in this topic before and after the trainings. The average pre-test score was 54%; the average post-test score was 90%. After the trainings, 95% of trainees reported high levels of confidence, knowledge and practical skill in this area. This is a significant improvement from the start of the training, when 67% reported a medium level of confidence, knowledge and skill and 28% reported low levels of confidence, knowledge and skill in this area.
Qualitative feedback from training participants reflected their experiences with the training and their thoughts on what they aimed do differently in their workplace as a result of the training. One of the Master Trainers said that she would “train different healthcare providers on importance of breastfeeding and assisting mothers to breastfeed.” A nurse who supports a district hospital neonatology unit said she would “use the [breastfeeding] checklist and incorporate it in neonatology daily work.” Another neonatology nurse commented that he would “teach the mother how to prepare the baby to breastfeed.”
Since that initial training, the Master Trainers have gone on to train an additional 70 health providers working across 10 district hospitals in all five provinces of Rwanda, reaching more than 4,400 mothers and babies to date. To ensure sustainability and consistent support for mothers in neonatal and post-partum units, a new hospital-based position was created, known as Expert Mothers. This position is now functioning in all three PIH-supported district hospitals in Rwanda with two Expert Mothers per hospital. Expert Mothers are women who previously had a child on the neonatology unit and now provide breastfeeding peer counselling to other mothers through mentorship, teaching and peer support to improve exclusive breastfeeding for infants needing care on neonatal units. The Expert Mothers received training from the Master Trainers at the start of their position and continued mentoring afterwards.
Prior to the WFID training and integration of Expert Mothers into hospital neonatal units, several other breastfeeding promotion interventions were introduced into the hospital neonatal and maternity units, including supplemental porridge to provide added nutrition to all mothers; water filters to ensure the availability of safe drinking water; breastfeeding u-shaped pillows for additional comfort and support while breastfeeding; breastfeeding corners where mothers could go to privately breastfeed or express breastmilk; and educational posters on the walls. Significant improvements were seen after the WFID training (March-July 2018) compared to the pre-training period (October 2017-February 2018) in the initial two hospitals where training was conducted: breastfeeding on the day of birth increased from 11.3% (n=37/237) to 26.9% (n=111/413, p<0.001); delayed introduction of breastmilk until two days or later after birth reduced from 49.6% (n=235/474) to 36.2% (n=193/533, p<0.001); and exclusive feeding from the breast at discharge increased from 63.1% (n=279/442) to 75.9% (n=441/581, p<0.001). There were non-significant trends of decline in neonatal unit mortality from 11.0% (n=61/493) of admissions to 8.1% (n=51/593, p=0.092) and no change in length of stay (mean of 10.4 days pre-training (n=554) and 10.5 days post-training (n=645, p=0.134) in the period immediately after training.1

Challenges and lessons learned
During the design process of the WIFD training programme, it was agreed that all trainees should have completed one of the WHO/UNICEF training courses on breastfeeding. However, it was evident that this was an unrealistic expectation. In most training settings, the nursing cadres had not received any formal breastfeeding training. The breastfeeding counselling sessions carried out daily in the KMC units and postnatal wards at the hospitals often did not follow WHO recommended guidelines. A lack of breastfeeding posters in relevant wards revealed further the limited rollout of WHO breastfeeding training material.
More than eighteen months after the trainings, the Master Trainers have reflected on what the WIFD training has taught them. Gato Saidath, a midwife, said that had she encountered a baby prior to the training with birth asphyxia who she “wouldn’t have been able to help feed on the breast,” and that, with the skills she has learned, she is now “able to try different positions.” She said that prior to the training “vulnerable babies suffered a lot.” Egide Karangwa, also a midwife, summed up the challenge he saw, saying, “As a midwife we are asked to put the baby on the breast soon after birth, but nobody told us how.” Since the training he is able to resolve issues of babies who are have difficulty breastfeeding, including alertness, attachment and identification of the root cause of a breastfeeding difficulty.
Next steps
This model of care, based on expert parent training, has been shown to be a successful strategy for longer-term sustainability in Rwanda (Palha et al, 2018). The Master Trainers in Rwanda will continue to provide mentorship to hospital neonatology and maternity unit-based staff, as will the six Expert Mothers who have been trained. While the Master Trainers have received remote support from the course directors of the training, an in-person post-training session is planned in the coming months to provide the opportunity for practical skills review with the course directors.
PIH plans to continue to monitor the impact of the WIFD training, including the Expert Mothers intervention, and seek opportunities to expand the reach of the Master Trainers, both within Rwanda and in other countries. Currently, the Master Trainers are leading ongoing research assessing the effectiveness of the breastfeeding interventions, including the WIFD training and the Expert Mothers. Further evaluation of the impact of the training on health outcomes for infants is required, as well as investigation into caregiver views on support received pre- and post-training.
MAITS receives regular requests for WIFD training to be carried out in neonatal and special care units in low- and middle-income settings. Not all settings meet the prerequisites for training that would enable successful implementation and rollout of the programme. Host organisations often struggle to coordinate logistics of organising a training programme. Most of these facilities, however, carry out KMC as part of their pre-term intervention package. WIFD has the potential to be integrated into KMC, which would enable more facilities to access targeted and evidence-based interventions. Scale-up of training programmes such as ENC and PCPNC has been less effective in comparison, and may not be the right platform to access the largest coverage at this stage. As Lawn et al (2013) point out, providing quality care involves doing the right thing at the right time. ‘Every Newborn: An Action Plan to End Preventable Deaths’ (WHO, 2014) identifies adapting KMC to make it deliverable at community level as a research priority. Incorporating safe feeding of vulnerable infants into the development of such a programme is likely to ensure long-term health benefits for the infants and service benefits for the health systems.
Currently, there are only two MAITS trainers delivering the initial training. However, it is envisaged that Master Trainers from low- and middle-income countries, rather than staff from developed countries, will go on to train others in countries in the region. The first such training is proposed between Rwanda and Liberia and hopefully between Rwanda and Uganda in the future. We believe that such a model will help rollout the training package to places where it is needed the most, using regional resources.
For more information please contact Himali de Silva and Maya Asir and to access the WIFD training please contact info@maits.org.uk
Endnotes
1Impact on length of stay and mortality of the training and other interventions is being examined to feature in future peer review publication (and Field Exchange summary).
References
Beck K, Kirk CM, Bradford J, et al. The Paediatric Development Clinic: A model to improve outcomes for high-risk children aged under five in Rural Rwanda. Field Exchange 58, September 2018. P51.
Christian P, Lee SE, Angel MD, et al. Risk of childhood undernutrition related to small-for-gestational age and preterm birth in low- and middle-income countries. Int J Epidemiol. 2013;42(5):1340-1355. doi:10.1093/ije/dyt109.
De Silva, H & Asir, M (2017) Working with infants with feeding difficulties: a training programme for healthcare staff in low-resource setting, MAITS, UK
Jadcherla S. Dysphagia in the high-risk infant: potential factors and mechanisms. The Am J Clin Nutr. 2016;103(2):622S-8S. doi: 10.3945/ajcn.115.110106.
Kakooza-Mwesige A, Tumwine JK, Eliasson A-C, Namusoke HK, Forssberg H. Malnutrition is common in Ugandan children with cerebral palsy, particularly those over the age of five and those who had neonatal complications. Acta Paediatr. 2015;104:1259-1268. doi: 10.1111/apa.13089.
Lawn JE, Kinney MV, Belizan JM et al. Born Too Soon: Accelerating actions for prevention and care of 15 million newborns born too soon. Reproductive Health. 2013, 10(Suppl 1): S6
Moxon S G, Lawn J E et al. Inpatient care of small and sick newborns: a multi-country analysis of health system bottle necks and potential solutions. BMC Pregnancy and Childbirth 2015, 15 (Supple 2): S7
Palha de Sousa, C., Beck, K., Kirk, C., Bradford, J., de Silva, H., Asir, M., Biziyaremye, F., Manirakiza, L., Saidath, G., Wilson, K., Karambizi, C.A. (2018). Promoting Early and Exclusive Breastfeeding for Vulnerable Infants with Feeding Difficulties in Neonatal Care Units in Rural Rwanda. Presented at American Academy of Pediatrics National Conference in Orlanda, Florida, 2-6 November 2018.
Rollins NC, Bhandari N, Hajeebhoy et al. Why invest and what it will take to improve breastfeeding practices. Lancet. 2016, 387(10017): 491-504
Thukral A, Lockyer J, Bucher S, Berkelhamer S, et al. Evaluation of an educational program for essential newborn care in resource-limited settings: Essential Care for Every Baby. BMC Pediatrics. 2015; 15:71
WHO, UNICEF. 2014. Every Newborn: an action plan to end preventable deaths. Geneva: World Health Organization.
WHO. Optimal feeding of low birth-weight infants in low-and-middle-income countries. Geneva, Switzerland. WHO; 2011 www.who.int/maternal_child_adolescent/documents/infant_feeding_low_bw/en/
WHO, UNICEF. Breastfeeding Counselling: A training course. Geneva, Switzerland. WHO;1993 www.who.int/maternal_child_adolescent/documents/who_cdr_93_3/en/
WHO, UNICEF. Infant and Young Child Feeding Counselling: An Integrated Course. Geneva, Switzerland. WHO; 2006 www.who.int/nutrition/publications/infantfeeding/9789241594745/en/
WHO (2019) Integrated management of childhood illness (IMCI) www.who.int/maternal_child_adolescent/topics/child/imci/en/
WHO. Kangaroo Mother Care: a practical guide. Geneva, Switzerland: WHO; 2003
WHO. Pregnancy, Childbirth, Postpartum and Newborn Care: A Guide for Essential Practice. 2nd ed. Geneva, Switzerland: WHO; 2006. www.who.int/maternal_child_adolescent/documents/imca-essential-practice-guide/en/
WHO. Essential newborn care course. Geneva, Switzerland: WHO; 2010 www.who.int/maternal_child_adolescent/documents/newborncare_course/en/
World Food Programme. Comprehensive food security and vulnerability analysis. Kigali, Rwanda; 2018.